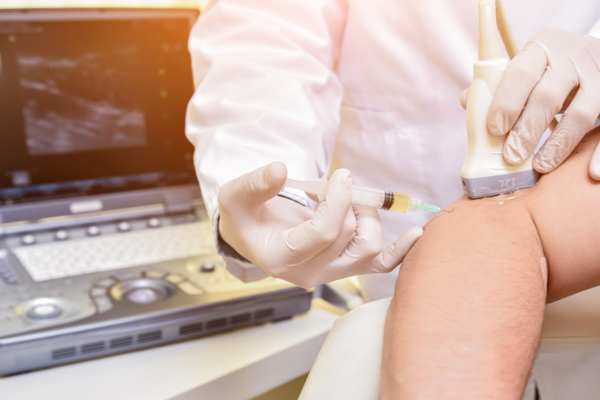
 Image-guided injections, such as epidural injections and facet joint blocks, offer a minimally invasive solution to address inflammation, pain and reduced mobility.
Image-guided injections, such as epidural injections and facet joint blocks, offer a minimally invasive solution to address inflammation, pain and reduced mobility.
A doctor may recommend this treatment after more traditional methods, such as medication or physical therapy, have not yielded significant results.
Injections without imaging technology have been used for years to address hip, shoulder and knee issues related to conditions like osteoarthritis, rheumatoid arthritis, ligament and muscle tears.
Cortisone, a local anesthetic or a joint lubricant like hyaluronic acid may be delivered to a specific spot to assist with pain management, improve mobility or reduce inflammation.
Imaging technologies, including ultrasound, computed tomography (CT) and fluoroscopy give this procedure a greater degree of accuracy, identifying the precise point of delivery.
Beyond pain management, this image-guided procedure may be used for joint aspirations, diagnostic purposes and to deliver stem cells or platelet-rich plasma to a particular area of the body. To assist with the procedure, imaging technologies provide real-time viewing of internal structures and deliver a greater degree of detail.
Without imaging, the technologist administering the injection often goes by touch, a less reliable method that may hit a nerve or blood vessel in the process. For these purposes, image-guided injections offer the following benefits.
1. Greater Accuracy
Image-guided injections allow the professional administering the dose to fully visualize the needle as it enters the joint and guide it to the precise location. Based on the imaging procedure, contrast dye may be used for an additional level of clarity.
Although traditional or “blind” injections are known to offer patients some relief they are not 100 percent accurate. With this technology, the accuracy rate jumps up over 90 percent due to real-time visuals and dynamic feedback that can be seen on the screen. As such, the imaging component allows doctors to observe the joint before and after the injection.
The ideal injection site may be just a few millimeters in size – nearly impossible to hit and identify without imaging of the body’s internal structures. Determining this location often results in greater pain relief for the patient.
Real-time imaging has another related benefit: Not only can the doctor administering the injection view the joint and surrounding structure to find the ideal path for the needle, but can also help avoid potential complications that may result from injecting a local anesthetic or pain reliever into the wrong spot.
2. Less Procedural Pain
An injection into the wrong area may simply numb it for a few hours – or could hit a nerve and cause the patient even more pain. In this regard, imaging technology greatly reduces this occurrence by identifying the most effective location to inject the medication. As a secondary benefit, it takes less time than a blind injection.
3. Lower Treatment Costs
For patients with hip osteoarthritis, an NIH study found that image-guided injections may lower healthcare costs long term. Although the procedure may cost more upfront, a single injection of hyaluronic acid to improve joint mobility lessened the amount of NSAID medications a patient used over the next two years by more than half. This pattern further reduces the number of NSAID complications a patient may experience.
4. A Higher Level of Detail
Image-guided injections may be performed with other imaging modalities, including fluoroscopy, CT scan or ultrasound, to provide detailed visualization of soft tissue structures, including tendons, nerves and blood vessels that the needle will need to navigate around.
On this note, the level of detail makes image-guided injections ideal for observing the fluid that accumulates around certain joints. In turn, this procedure can help treat patients living with bursitis, arthritis, neck and pack pain, tendinopathy and sciatica while reducing potentially painful, life-threatening complications.
Has your doctor recommended an image-guided injection? Contact Midstate Radiology Associates to make an appointment today.












